Research Shows Poppers Causes Damage to the Eye
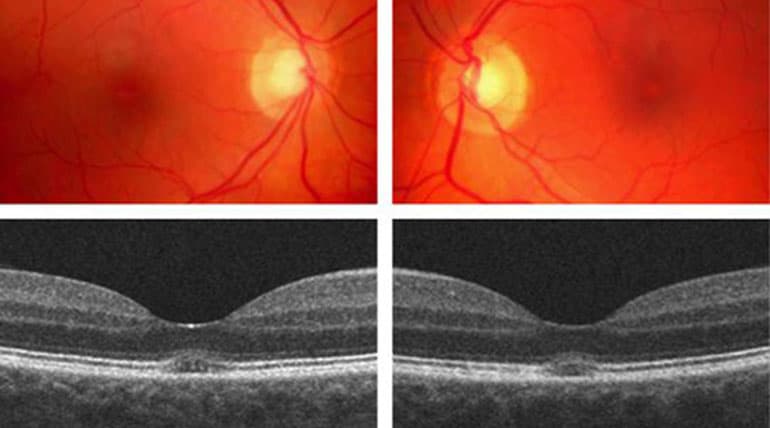
A 38-year-old man was referred to the medical retina service for evaluation of bilateral macular lesions noted by his general ophthalmologist. Medical history was otherwise unremarkable. On examination, his best-corrected visual acuity was 20/20 OU, although his vision was slightly eccentric. His pupils were round and reactive. The slitlamp examination of the anterior segment was unremarkable. Dilated fundus examination revealed subtle bilateral yellow foveal spots. Optical coherence tomography (OCT) displayed the presence of a bilateral foveal defect of the external limiting membrane and ellipsoid zone bands.
Poppers is a term for the chemical class of alkyl nitrites, which are inhaled for recreational drug purposes, typically for the high or rush that the drug may produce. Poppers have also been historically used by men who have sex with men for their ability to relax the anal sphincter. Although poppers are illegal, they can be purchased in some countries as alternative products, which include room deodorizers or video head cleaners. The use of poppers is thought to be high and ranges between 5% to 6% in French teenagers and up to 10% of adults in the United Kingdom. However, their use may be higher in certain groups and is estimated to be about 60% in Australia’s gay community.
While the exact mechanism causing damage of the central photoreceptors is still uncertain. Researchers have suggested that alkyl nitrites may cause an increase in nitric oxide. Nitric oxide exposure is known to raise intracellular cyclic guanosine monophosphate levels, eventually causing photoreceptor apoptosis.

A possible association between the use of poppers and maculopathy was first proposed in 2004. After this first description, several reports have characterized this clinical entity. In detail, ophthalmoscopy findings can be very subtle, with more striking changes seen on OCT, which may show either a hyperre-flective or hyporeflective ellipsoid zone band. Although OCT changes associated with poppers maculopathy have been thus characterized, these alterations are not specific for this maculopathy. As an example, solar maculopathy may be characterized by similar changes at the fovea. Furthermore, similar foveal abnormalities may occur after blunt ocular trauma and whiplash injury. For these reasons, when a patient presents with a localized alteration of the foveal photoreceptors, a focused drug history of the patient is mandatory. Nonetheless, the diagnosis can be complicated by patient denial of popper use. Noteworthy, the use of poppers was suggested to produce a dose-related increase in photoreceptor damage, with individuals with long-term regular use showing most severe macular alterations.
The relatively easy availability of poppers has increased their popularity as recreational drugs. Lesions occurring in poppers maculopathy are frequently permanent and may be associated with a substantial effect on vision. This case highlights the importance of obtaining an in-depth medical and personal history of patients presenting with a focal damage of the foveal photoreceptors. In this case, the patient revealed his recreational use of different drugs, including poppers, cannabis, and cocaine, for approximately 15 years.
Prescribing laboratory testing to investigate causes of intraocular inflammation (choice A) would not be preferred because a bilateral foveal photoreceptor loss is an uncommon presentation for uveitis, especially in a patient without other ocular signs of inflammation. A dye angiography (choice B) was not recommended as the next step because no other retinal and/or choroidal alterations were evident on spectral-domain OCT images. Treating the patient with antiviral drugs (choice D) would not be the next recommended step because of the absence of a viral infection.
Patient Outcome
The patient was extensively informed about his condition and the prognosis. Moreover, he was screened for HIV, as many patients with poppers maculopathy were reported to be affected by this infection, and the result was negative. Importantly, he was advised to discontinue the use of poppers and to follow up with a medical retina specialist. His vision and foveal lesions remained stable throughout the 1-year follow-up.
References: JAMA Ophthalmology Clinical Challenge