Click here to resize type
Diabetic Retinopathy Treatment in West Palm Beach & Jupiter, FL
If you have diabetes, you probably understand the health repercussions of the disease to your heart, kidneys and nerves. But you may not be familiar with the risks to your eyes. Diabetes is a risk factor for ocular diseases like glaucoma and cataracts. If your blood sugar levels get too high, diabetic retinopathy, wherein the small blood vessels of the eyes swell, leak or even stop functioning completely, can occur.
At later stages of diabetic retinopathy, the retina actually grows new blood vessels, which leak blood into the eye’s vitreous fluid. The new vessels can also form scar tissue that may lead to the development of a detached retina. The end result of all of these changes is often the partial or complete loss of eyesight.
How Diabetic Retinopathy Affects the Eyes
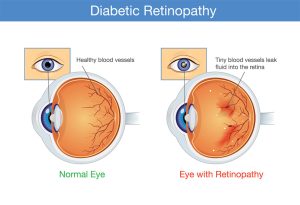
Sustained high blood sugar levels can damage the blood vessels at the back of the eye in the retina. In addition to making the blood vessels leak blood, new vessels that are abnormal and similarly leaky may grow. This impacts the retina’s ability to send messages to the brain via the optic nerve and may cause irreversible vision loss or total blindness. Diabetic retinopathy can also be a precursor to other devastating eye conditions like glaucoma, retinal detachment, and macular edema.
About one in three adults (middle age and older) who have diabetes go on to develop diabetic retinopathy. It is one of the leading causes of permanent blindness in the United States.
Symptoms of Diabetic Retinopathy
Patients who have diabetic retinopathy may experience symptoms such as:
- Blurry vision
- Discomfort or pain in the eye
- Floaters (spots or lines that float through the field of vision)
- Diminished ability to see at night
- Red eyes
- Occasional but inconsistent vision loss
- Dark or vacant spots in your vision
- Increased difficulty discerning colors
Diagnosing Diabetic Retinopathy
Early on, diabetic retinopathy’s symptoms may be more difficult for a patient to recognize. That makes it especially important for patients with diabetes to undergo periodic comprehensive eye exams to diagnose diabetic retinopathy — before it has a chance to permanently rob their vision.
The test for diabetic retinopathy requires dilating the pupils. This allows the eye doctor to see the back of the patient’s eye more easily and identify any abnormalities that could pose a problem. Potential red flags include scar tissue on the retina, blood in the vitreous, newly formed blood vessels, and irregularities of the optic nerve.
If the first test reveals signs of diabetic retinopathy, further tests are administered, such as optical coherence tomography (OCT), which generates images of the patient’s retina. Here, a doctor can measure the retina’s thickness with these pictures, which is an indication of how much fluid has leaked into the retinal tissue. Additionally, fluorescein angiography can help pinpoint the specific vessels in the retina that are leaking blood.
Individuals At Risk for Diabetes
Overweight individuals are at the most serious risk for developing type 2 diabetes. Type 1 diabetes, which is usually attributed to genetic factors or autoimmune disease, only accounts for 10 percent or less of diabetes cases. Type 2 diabetes is linked to excess body weight, which increases blood sugar levels and triggers insulin resistance. This puts an enormous strain on the pancreas to produce enough insulin.
Some cases of type 2 diabetes are caused by genetic factors; however, the chances of getting it greatly increase if you are obese and/or physically inactive. The higher your body mass index (BMI), the greater your chances of getting type 2 diabetes.
How do we know this? When type 2 diabetics increase their physical activity levels and lose weight, their diabetes either improves or goes away completely.
Diabetic Retinopathy Treatment Options
The best protection against diabetes-related eye problems is to target the root of the problem: diabetes. Our eye doctors highly recommend managing diabetes by taking your medications as prescribed, seeing your medical team regularly, eating a healthy diet and exercising regularly.
If diabetic retinopathy becomes more serious for a patient, urgent medical treatment is appropriate. Mittleman Eye offers multiple treatment options:
VEGF Inhibitors
VEGF (vascular endothelial-growth factor) inhibitors are medications that are injected into the vitreous (the gel-like fluid between the lens and the retina) to alleviate existing fluid accumulation and stop the retina from generating new, faulty blood vessels. Regular injections are necessary to maintain the results, but this treatment method is highly safe and effective. In fact, nearly 90% of patients have found success in stabilizing their vision with anti-VEGF drugs like Avastin, Lucentis, and Eyelea.
Focal Laser Treatment
In a process also known as photocoagulation, an ophthalmologist can use a laser to seal faulty blood vessels to either stop or dramatically slow the rate at which blood leaks into the eye. For many patients, laser treatments have also been found effective at blocking new blood vessel growth.
Vitrectomy
This surgery involves removing the liquid in the vitreous so that the ophthalmologist can eliminate any excess blood and scar tissue that formed due to diabetic retinopathy. Once this process is complete, the doctor replaces the vitreous with a synthetic fluid.
Nutrients and Fiber to Manage Diabetic Retinopathy
Evidence suggests that increasing your fiber consumption helps your body manage your blood sugar levels. High-fiber foods also help you feel fuller on fewer calories.
A diet rich in key vitamins and minerals strengthens your eyes and helps prevent ocular diseases. Among the best nutrients are omega-3 fats, beta carotene, lutein, zeaxanthin and zinc. Vitamin A, B vitamins, iron and thiamine are essential for your eyes. Non-starchy plant foods, such as fruits and leafy vegetables, are ideal sources of vitamin B. This eye-healthy vitamin can also be found in whole grains, eggs, dairy products, meat, nuts, seeds and legumes. Daily vitamin supplements are a good idea for those who do not consume sufficient amounts of these nutrients.
Exercise, too, is an important way to prevent and manage diabetes. Vigorous physical activity helps your system control glucose and strengthens the pancreas.
Schedule a Consult for Diabetic Retinopathy
If you would like to learn more about diabetes and diabetic retinopathy, we invite you to schedule a personal consultation with an experienced ophthalmologist at our West Palm Beach or Jupiter office by contacting Mittleman Eye today.
















